CLINICAL STUDIES
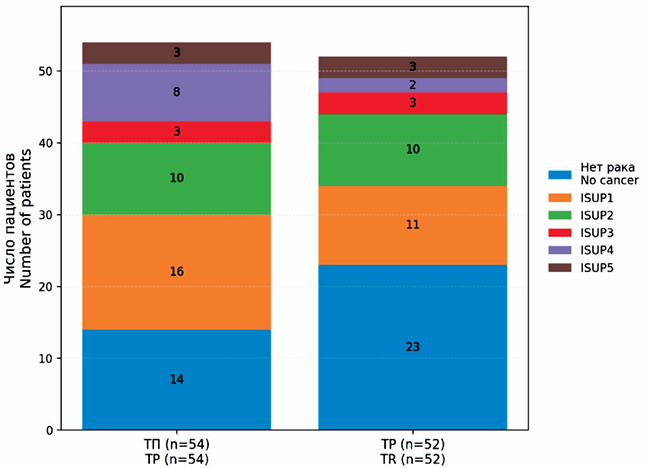
Objective: to compare transperineal (TP) versus transrectal (TR) prostate biopsy under local anesthesia in terms of diagnostic yield, safety, and patient tolerability in an outpatient randomized trial.
Material and Methods. A total of 106 men with suspected prostate cancer were randomized 1:1 to TP (n=54) or TR (n=52) biopsy. All patients underwent 12-core systematic sampling; MRI-targeted cores were added for PI-RADS ≥3. Antibiotic prophylaxis was given only in the TR group. The primary endpoint was detection of clinically signifcant prostate cancer (csPCa, ISUP ≥2). Secondary outcomes included overall cancer detection, complications (Clavien–Dindo), pain scores (VAS), procedure time, and satisfaction.
Results. Cancer was detected in 74.1 % of TP vs 55.8 % of TR patients (p=0.066). csPCa was found in 44.4 % vs 34.6 % (p=0.33). Infectious complications occurred only after TR biopsy (11.5 % vs 0 %; p=0.012). No severe (grade III–V) events were observed. Minor events (hematuria, hematospermia) occurred in 30 % of both groups. Median VAS pain was lower in TP (3 vs 5, p<0.01); severe pain (VAS ≥6) was reported by 6 % in TP vs 33 % in TR. Median procedure time was longer with TP (20 vs 8 min, p<0.001). Patient satisfaction was high in both arms (85 % vs 75 %, p=0.20).
Conclusion. Outpatient TP biopsy provided equivalent diagnostic performance to TR, with markedly fewer infectious complications and lower pain scores. Despite longer procedure time, satisfaction remained high. These fndings support TP biopsy as a safer alternative to TR in routine practice.
The aim of this study was to evaluate the diagnostic and prognostic potential of QClamp™ real-time PCR technology for the detection of ctDNA carrying KRAS gene mutations in patients with pancreatic ductal adenocarcinoma.
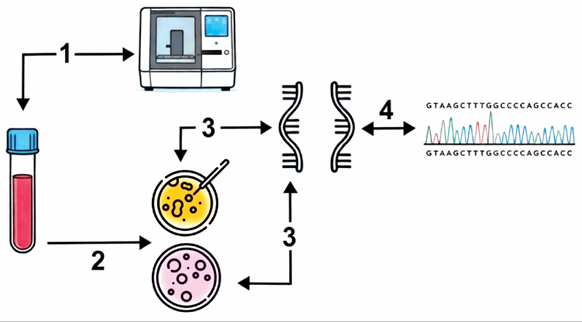
Material and Methods. The study included 119 patients with different stages of pancreatic cancer. Cell-free DNA was isolated from blood plasma, and the most common somatic KRAS mutations were detected using XNA-mediated suppression of wild-type DNA amplifcation.
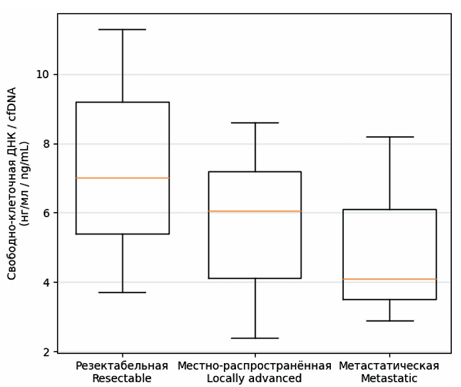
Results. KRAS mutations in plasma were identifed in 23.5 % of patients, with the detection rate of ctDNA increasing with disease progression, reaching 66.7 % in locally advanced disease and 25.0 % in metastatic pancreatic cancer. In patients with resectable stages (I–II), ctDNA was detected in only 15.6 % of cases; however, its presence was associated with signifcantly worse overall survival and recurrence-free survival. The concentration of total cell-free DNA varied substantially and did not directly correlate with disease stage, indicating the limited informative value of this parameter in the absence of molecular analysis.
Conclusion. The results obtained demonstrate that QClamp™ PCR is a rapid and technically feasible method for ctDNA detection with high specifcity. The greatest clinical applicability of this technology may lie in prognostication and monitoring of minimal residual disease after surgical treatment, complementing existing clinical and instrumental approaches.
Introduction. Parameningeal rhabdomyosarcoma with intracranial spread is a highly aggressive pediatric malignancy with a high risk of leptomeningeal metastasis. Historically, central nervous system (CNS) involvement was considered an incurable condition with a survival rate of no more than 10–20 %. The bloodbrain barrier is the primary barrier to the penetration of most drugs and the creation of effective concentrations. Therefore, the search for effective and non-toxic methods for controlling leptomeningeal metastases is one of the most pressing challenges in pediatric oncology. Intrathecal chemotherapy (ITCT) delivers cancer drugs directly into the cerebrospinal fuid, bypassing the BBB. It enables high concentrations of medication to directly target cells, reducing systemic toxicity.
The purpose of the study was to evaluate the effcacy and safety of intrathecal chemotherapy in a multidisciplinary approach to the treatment of children with parameningeal rhabdomyosarcoma with intracranial spread and/or leptomeningeal metastasis, and to improve survival rates in this cohort of children.
Material and Methods. The study included 21 patients with a histologically verifed diagnosis of parameningeal rhabdomyosarcoma with intracranial spread and/or leptomeningeal metastasis, who received treatment at the L.A. Durnov Research Institute of Pediatric Oncology and Hematology of the Russian Academy of Medical Sciences from 2021 to 2024. The study was approved by the local ethics committee.
Results. With a 34.3-month median follow-up, the overall 2-year survival rate was 65 %. This indicates the effectiveness of early tumor control by overcoming the blood-brain barrier. The overall 2-year survival rate was signifcantly higher in both the prophylactic and therapeutic frst-line intrathecal chemotherapy groups than in the relapse group (80 % vs 20 %, p<0.05) and signifcantly exceeded the median survival time of 4–6 months reported by other authors [1]. The toxicity profle of ITCT was favorable, with no cases of severe neurotoxicity.
Conclusion. Intensive intrathecal chemotherapy in the combination treatment of children with parameningeal rhabdomyosarcoma with intracranial extension and/or leptomeningeal metastasis is an effective and safe method for treating and preventing CNS tumor cell infltration. This therapy can signifcantly improve survival of patients with extremely unfavorable prognosis.
LABORATORY AND EXPERIMENTAL STUDIES
Germline pathogenic variants in DNA repair genes (BRCA1/2, RAD50, RAD51D, PTEN and etc.) are responsible for the development of hereditary breast and ovarian cancers. The large number of variants detected by NGS technology have unknown or conficting clinical signifcance. Reclassifcation of these variants plays a crucial role in their application in routine laboratory practice.
The aim of the current study was to reclassify conficting RAD51D gene variant (rs145309168) in a young Buryat breast cancer patient using the translation-dependent nonsense-mediated mRNA decay (NMD) pathway.
Material and Methods. Wholeexome sequencing (WES) was performed in the germline DNA of 16 non-BRCA BC Buryat patients (data not shown). The diagnosis in all patients was confrmed morphologically (T1–3N0–2M0). All tested women were diagnosed with invasive (ductal) carcinoma of no special type. Rare variants (MAF<0.005) were analyzed to assess their impact on the RNA splicing using in silico tools like SpliceAI, ESEFinder, RESCUE-ESE, and EX-SKIP. A rare missense variant in the RAD51D gene (rs145309168) was identifed in a 39-year-old Buryat breast cancer patient. Frozen patient leukocytes were divided into experimental and control samples. The samples were cultured for 5–6 days and treated with puromycin (only experimental samples) for 4–6 hours prior to RNA isolation to avoid NMD followed by Sanger sequencing.
Results. In vitro experiments on live leukocytes from a breast cancer patient with the c.932T>A variant of the RAD51D gene were conducted. cDNA amplicons were obtained from RNA isolated from control and experimental leukocytes (treated with puromycin to avoid nonsense-mediated decay). For an accurate assessment of splicing aberrations, transcripts from the experimental leukocytes were compared to transcripts from control leukocytes by using Sanger sequencing. In both cases, the presence of the studied variant in the RNA signifed that the variant did not activate NMD and therefore did not affect splicing.
Conclusion. This study presents the frst in vitro functional analysis of the RAD51D variant (rs145309168) identifed in a young Buryat breast cancer patient. Our experimental data demonstrate that this variant does not disrupt normal splicing, providing evidence for its reclassifcation as «Likely Benign», which is consistent with published data and previous classifcations.
Background. Colorectal cancer (CRC) is characterized by high mortality and the development of therapy resistance. Indole-3-propionic acid (IPA), a gut microbiota-derived metabolite, shows promise in treating colorectal cancer (CRC) by strengthening antitumor immunity and improving chemotherapy effcacy.
The aim of the study was to evaluate the antitumor activity of indole-3-propionate in vivo using a mouse model of colorectal cancer.
Material and Methods. The experiment was conducted on 42 female mice with subcutaneous CT26 CRC. After reaching a tumor volume of 50–60 мм3 , the animals were randomized into 6 groups (n=7): control (0.9 % NaCl saline i.p. and p.o.), IPA monotherapy (6 mg/kg, p.o.), 5-fuorouracil (5-FU) (25 mg/kg, i.p.), oxaliplatin (OXA) (10 mg/kg, i.p.), combination IPA (6 mg/kg, p.o.) + 5-FU (25 mg/kg, i.p.) and IPA (6 mg/kg, p.o.) + OXA (10 mg/kg, i.p.). Drugs were administered 3 times per week (Mon, Wed, Fri) for 3 weeks. The results were assessed one week after the end of treatment. Tumor volume and tumor growth inhibition (TGI) percentage were evaluated. Statistical analysis was performed using the Mann-Whitney U-test.
Results. IPA monotherapy had no signifcant effect (TGI=5.0 %). Chemotherapeutic agents in monotherapy demonstrated moderate activity: TGI 22.9 % for 5-FU and 19.4 % for OXA. The greatest effcacy was achieved in the combination therapy groups: TGI 31.9 % for IPA + 5-FU and 30.1 % for IPA + OXA. Statistically signifcant growth inhibition in these groups was registered from day 18 (4 days earlier than with cytostatic monotherapy). Toxicity, assessed by body weight dynamics, was absent in all groups.
Discussion. The results obtained demonstrate that IPA does not possess independent cytotoxic activity against CT26 tumor cells. However, its potential in combination with standard chemotherapeutic drugs was revealed. Earlier and more pronounced TGI in the combination therapy groups indicates the ability of IPA to accelerate the development of a therapeutic response.
Conclusion. IPA potentiates the antitumor activity of 5-FU and OXA on the CT26 CRC model without increasing systemic toxicity. The obtained data justify further study of the mechanisms of IPA synergy with chemotherapeutic agents and its effcacy in other malignant neoplasms.
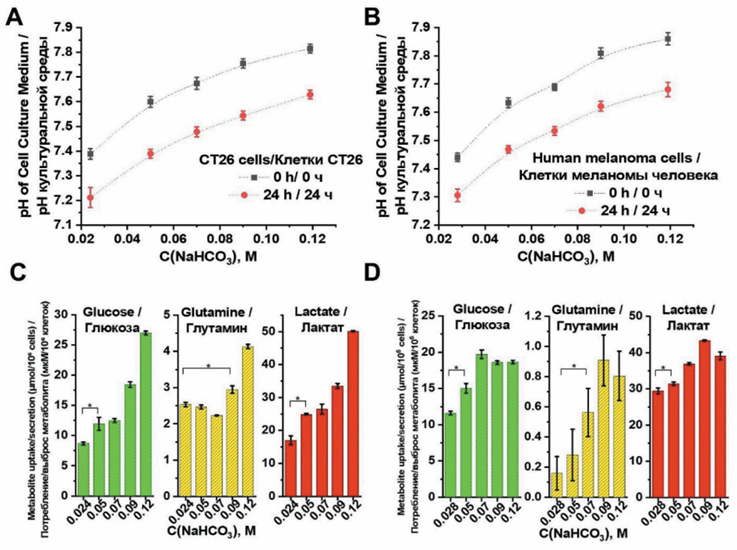
Tumor microenvironment acidity represents a fundamental hallmark of cancer that promotes tumor progression, invasion, immune evasion, and treatment resistance.
Objective. This study investigates the antitumor mechanisms of sodium bicarbonate-induced alkalization on mouse colon adenocarcinoma CT26 cells and human melanoma cells.
Material and Methods. Cells were treated with varying sodium bicarbonate concentrations (50–119 mM) to assess effects on viability, metabolism, migration, and cell death pathways.
Results. Results demonstrated immediate concentration-dependent extracellular pH elevation that decreased after 24 hours due to metabolic adaptation. Both cell lines exhibited dose-dependent cytotoxicity with an IC50 of approximately 80–90 mM, yet minimal apoptosis was detected via Annexin V/PI staining, suggesting alternative cell death mechanisms. Sodium bicarbonate signifcantly impaired cellular migration in wound healing assays, coinciding with mitochondrial depolarization as evidenced by reduced Mito Red fuorescence. Metabolic analysis revealed increased consumption of glucose and glutamine alongside elevated lactate production, indicating metabolic reprogramming in response to alkalization stress. While lysosomal accumulation increased with treatment (measured by Lyso Green), canonical autophagy markers (LC3B and p62) showed no signifcant changes, suggesting classical autophagy pathways are not primarily involved.
Conclusion. These fndings indicate that sodium bicarbonate-induced alkalization triggers tumor cell death through mechanisms beyond conventional apoptosis and autophagy, potentially involving lysosome-mediated cell death or alkaliptosis. The study provides mechanistic insights supporting sodium bicarbonate as a potential adjuvant therapy that targets the tumor microenvironment’s acidity, with implications for enhancing conventional cancer treatments through pH modulation. Further research is needed to fully elucidate the precise cell death pathways involved.
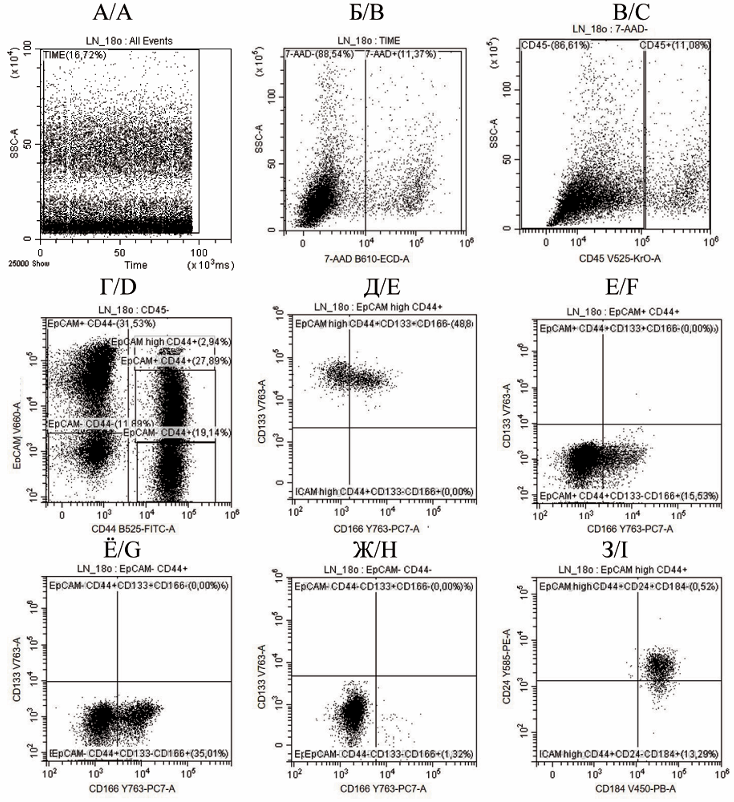
Background. Cancer stem cells (CSCs) are considered to be responsible for progression and recurrence of colorectal cancer (CRC). A detailed study of the phenotype of these cells and their immunobiological properties is necessary for developing CRC treatments. The aim of the study was to assess the percentage of EpCAMhigh/CD44+ cancer stem cells in colorectal cancer and to detect the expression of CD133, CD166, CD24 and CD184 on their surface.
Material and Methods. A one-stage cross-sectional study of the cellular composition of tumor tissue was performed in 123 patients with stage III colon adenocarcinoma. The control group consisted of 87 patients who underwent surgery for non-neoplastic diseases of the colon. An enzymatic method was used to obtain a suspension of tumor tissue cells. Gating of non-lymphoid cells (CD45-) was performed depending on the expression of the epithelial cell adhesion molecule EpCAM and the differentiation antigen CD44 on their surface. Expression of EpCAM, CD44, CD133, CD166, CD184 and CD24 on CSCs was studied by fow cytometry.
Results. The CD45-EpCAMhighCD44+ colorectal cancer stem cells (CSCs) accounted for 17.15 % [11.76; 26.44] of the non-lymphoid cell population. Within this CSC population, 42.83 % [37.07; 51.77] simultaneously expressed CD133 and CD166, while 57.17 % [48.23; 62.93] expressed the CD133 antigen alone. All CSCs in the primary tumor expressed CD184, and 95.18 % [88.48; 97.98] of them simultaneously expressed CD24. The percentage of EpCAMhighCD44+ cells in well-differentiated tumors was 1.5 times lower than that in moderately-differentiated tumors (U=326.5, p=0.002) and 2.1 times lower than in poorly-differentiated tumors (U=21.0, p<0.001). In addition, the percentage of EpCAMhighCD44+CD133+CD166+ cells in stage IIIC CRC was 13 % higher than that in stage IIIB CRC (U=1116.0, p=0.007).
Conclusion. In primary colorectal cancer tumors, cancer stem cells expressing high levels of EpCAM and CD44 accounted for 17.2 % of the non-lymphoid cell pool. The percentage of EpCAMhigh/CD44+ cells in poorly differentiated tumors was higher than that in well-or moderately-differentiated tumors.
Background. Expression of the main mediators of infammatory signaling – cytokines and long non-coding RNAs (lncRNAs) – determines the course of the tumor process and the formation of a platinum-insensitive phenotype in ovarian cancer.
The aim of the study was to evaluate the co-expression of long non-coding RNAs HOTAIR, MALAT1, PVT1 with proinfammatory cytokines in blood plasma during the formation of a platinum-insensitive phenotype in ovarian cancer.
Material and Methods. The study included 46 patients with primary ovarian cancer treated at the Ulyanovsk Oncology Center in 2018–2020. RNA was isolated from 2 ml of patients’ blood plasma before treatment, followed by reverse transcription and polymerase chain reaction to analyze the expression of HOTAIR, MALAT1, and PVT1. Plasma levels of the cytokines IL-1β, -10, -17A, and -18 were also determined. Ovarian cancer patients were divided into 2 groups based on the duration of the platinum-free interval.
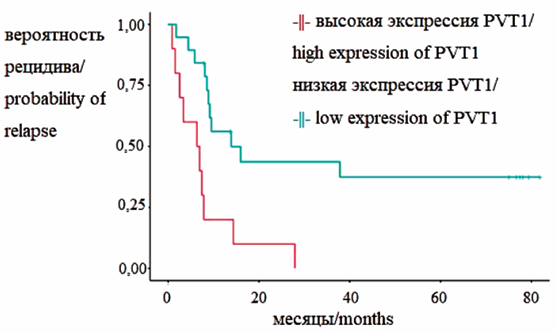
Results. Plasma expression of long non-coding RNAs (lncRNAs) HOTAIR, MALAT1, and PVT1 was found to be signifcantly higher in patients with ovarian cancer than in patients with benign ovarian tumors. Plasma HOTAIR expression was also higher in stages III–IV ovarian cancer compared to stages I–II. Patients with platinum-insensitive ovarian cancer had signifcantly lower levels of IL-17A and IL-10 compared to patients in the comparison group, but higher levels of IL-1β and IL-10 compared to patients in the platinum-sensitive group. A correlation was found between the levels of lncRNA MALAT1 and IL-18.
Conclusion. The serum expression level of PVT1 lncRNA in ovarian cancer patients correlates with progression-free survival and allows for assessing the likelihood of disease recurrence. Serum coexpression of MALAT1 and IL-18 lncRNAs can be used as a predictive marker for identifying platinuminsensitive ovarian cancer. Their combined overexpression with proinfammatory cytokines and IL-1β before chemotherapy has prognostic potential as a marker of platinum resistance in ovarian cancer. A prognostic model for assessing the risk of cancer progression in the frst 6 months after diagnosis includes MALAT1 and HOTAIR expression data at the start of therapy and serum IL-1β and -18 levels. A K-value above 1.65 indicates a high risk of disease progression.
ONCOLOGY PRACTICE
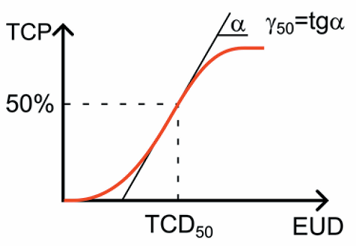
Background. Radiotherapy is one of the primary methods for treating malignant neoplasms, and its effectiveness depends on the ratio of radiation doses absorbed by tumor and healthy cells. The quality of a dosimetric plan is traditionally assessed based on physical and dosimetric criteria; however, radiobiological aspects should be taken into account to achieve the maximum predicted therapeutic effect. The existing variety of radiobiological models and the lack of a unifed approach to systematizing their numerical parameters hinder their practical application, making the creation of a specialized database a relevant task.
Objective: to develop a database of clinically signifcant radiobiological parameters for tumors and normal tissues for photon and neutron therapy as a unifed specialized tool to improve the accuracy of dosimetric planning and predict clinical treatment outcomes for malignant neoplasms.
Material and Methods. An analysis of more than 100 scientifc publications from open sources dedicated to the calculation of clinically signifcant radiobiological parameters of widely used radiobiological models was conducted. During the study, data were systematized considering various fractionation regimens, radiation energy and type, radiotherapy techniques, localization and volume of the irradiated area, as well as individual patient characteristics.
Results. A database of clinically signifcant radiobiological parameters for photon and neutron therapy was created. Based on the structured data, a web application was developed using the Python and JavaScript programming languages. The web application is integrated into the “TCP/NTCP Calculator” software and provides capabilities for storage, rapid search, and analysis of radiobiological parameters.
Conclusion. The created database systematizes clinically signifcant radiobiological parameters and provides specialists with a unifed tool for predicting probable treatment outcomes and assessing the risk of adverse effects on critical organs and tissues. This tool can be used in clinical practice, educational programs for training specialists in medical physics and radiotherapy, as well as for the in-depth study of radiobiological effects and the development of new treatment methods.
REVIEWS
Objectives: to conduct a systematic review of current data on breast cancer epidemiology and risk factors; to develop a clinical profle of young breast cancer patients and describe approaches to their treatment and rehabilitation; to develop a prevention strategy for high-risk groups.
Material and Methods. A search was conducted in the Web of Science, PubMed, Scopus, and Google Scholar databases. The review incorporated 60 sources (systematic reviews, meta-analyses, randomized clinical trials). A comparative analysis of risk factors, clinical presentation, diagnosis, treatment, and rehabilitation of young breast cancer patients compared to elderly patients was conducted.
Results. Breast cancer poses a signifcant health challenge for women aged under 40 years, representing the second leading cause of cancer-related mortality in this age group worldwide. A trend towards an increase in breast cancer incidence is observed among young women. The lack of tailored breast cancer screening for young women causes signifcant diagnostic delays, leading to late-stage cancer at detection, negatively impacting clinical outcomes and increasing the risk of treatmentrelated complications compared to elderly patients. Pathomorphology of tumors detected in young women is characterized by poorly differentiated cells, increased Ki67 expression, the presence of gene mutations, and a predominance of HER2-positive and triple-negative immunohistochemical subtypes. Despite these evident differences, research on breast cancer in young women remains insuffcient, creating gaps in understanding its risk factors, diagnosis, prognosis, and treatment. A lack of age-specifc clinical data and outcomes hinders the adaptation of standard treatment approaches, developed for elderly patients, to the needs of young women.
Conclusion. Further research is needed to collect age-specifc clinical data and develop novel treatment strategies for breast cancer in young women, ultimately improving treatment outcomes and identifying promising research directions in this area.
The aim of the study was to systematize current data on the use of human epididymis protein 4 (HE4) as a tumor-associated marker for lung cancer (LC) diagnosis, prognosis of treatment response, and monitoring of this category of patients.
Material and Methods. A search and analysis of available Russian and Englishlanguage sources was performed in the RSCI and PubMed databases using keywords “lung cancer” and “HE4”. The review includes 44 papers published between 2006 and 2024.
Results. HE4 is involved in gynecological cancer progression, but its role in the development of LC remains poorly studied despite its high expression in tumor tissue. Modern studies demonstrate that diagnostic characteristics of serum HE4 are comparable to or slightly superior to other markers used in the diagnosis of LC (CYFRA21-1, CEA, NSE, ProGRP, etc.). Several studies report that the HE4 serum level can serve as a predictor of response to chemotherapy and the duration of the relapse-free interval in LC. Some studies indicate the feasibility of HE4 as a marker for monitoring patients for early detection of lung cancer relapse. The indicators of the diagnostic and prognostic signifcance of serum HE4 vary signifcantly in different studies due to the heterogeneity of the included groups, differences in the reference values and methods for assessing the HE4 levels. This does not allow us to adopt a unifed diagnostic algorithm for using HE4.
Conclusion. The accumulated data indicate the feasibility of using HE4 as a tumor-associated marker in LC. However, some aspects that are important for the practical application of HE4 remain unclear. Thus, the introduction of this marker into clinical practice requires further systematic and in-depth studies.
Background. Over the past decade, the understanding of the biology of HER2-negative breast cancer has changed signifcantly due to the identifcation of the HER2-low and HER2-ultralow categories, which have gained clinical signifcance with the advent of new-generation antibody-drug conjugates.
Goal: to systematize recent data on the molecular and morphological features of this group of tumors, discuss the diagnostic diffculties associated with interpreting low levels of HER2 expression, and provide data from key clinical studies that have determined the role of ADC in the treatment of patients with HER2-low and HER2-ultralow breast cancers.
Material and Methods. The literature search was conducted in Medline, Cochrane Library, and Elibrary databases, covering the period from 2004 to 2025.
Conclusion. HER2-low and HER2-ultralow breast cancers represent clinically signifcant subtypes, presenting diagnostic and therapeutic challenges. Further studies are needed for refning diagnostic criteria and developing targeted therapies.
Objective: to analyze current approaches to the assessment of biochemical markers of skeletal muscle metabolism, to identify promising research directions in this feld, and to outline potential therapeutic strategies.
Material and Methods. The literature search for the preparation of the review was conducted using the Web of Science, Scopus, MEDLINE, Cochrane Library, RSCI, and PubMed databases. A total of 146 sources were analyzed, of which 47 scientifc publications were selected. The review includes studies published between 2010 and 2025.
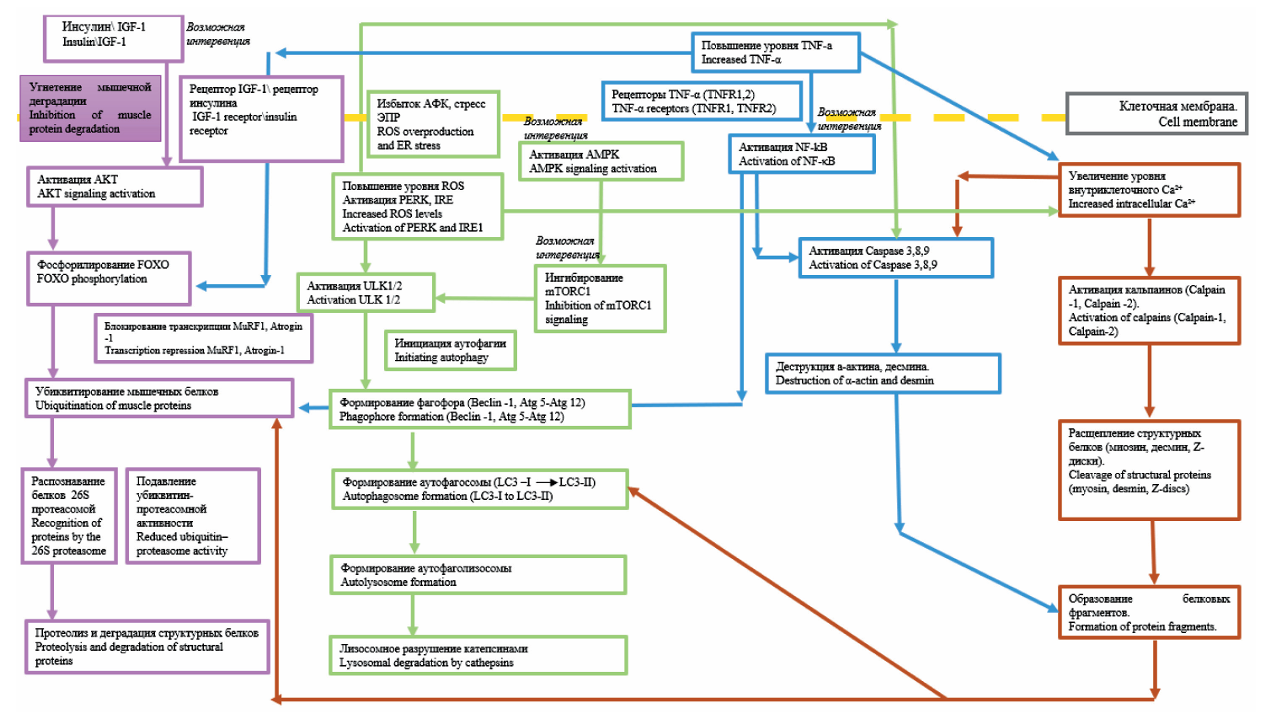
Results. Sarcopenia in cancer patients involves four key proteolytic cascades: the ubiquitin– proteasome pathway, autophagic pathway, calpain-dependent pathway, and caspase-dependent pathway. Particular attention was given to the prognostic role of biochemical markers, including muscle-specifc E3 ligases (MuRF1, Atrogin-1), infammatory cytokines, and cystatin C. A high prognostic value of the creatinineto-cystatin C ratio was demonstrated for assessing the risk of anticancer therapy toxicity and mortality. Promising molecular targets, such as AMPK, IGF-1/AKT/mTOR, and the NF-κB, were identifed for targeted therapy.
Conclusion. Sarcopenia in cancer arises from complex and molecular mechanisms, including both protein degradation and impaired muscle tissue regeneration. The use of biochemical markers and targeted interventions opens up prospects for precise, personalized medicine, enabling earlier diagnosis, accurate prognosis, and tailored treatments. Further clinical studies are required to validate biomarkers and evaluate the effectiveness of novel therapeutic strategies aimed at preventing muscle atrophy in cancer patients.
Background. Prostate cancer is a leading malignancy among men worldwide, presenting signifcant public health challenges due to its complex biology and diverse clinical outcomes. Recent advances in bioinformatics have greatly infuenced cancer research by enabling the integration of multiple disciplines and improving the analysis of biological data.
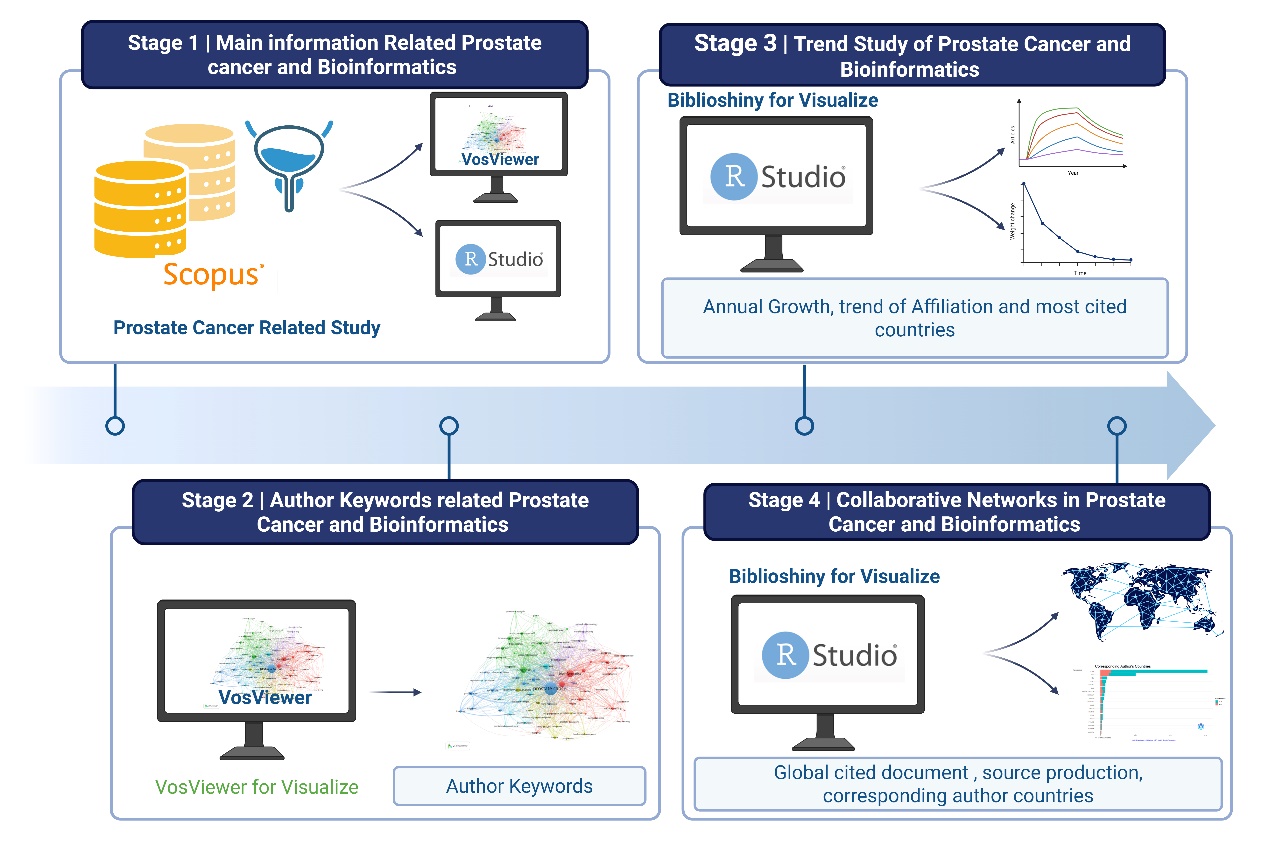
Objective. To present a comprehensive bibliometric analysis summarizing global research trends in prostate cancer and bioinformatics from 1998 to 2025.
Material and Methods. A bibliometric study was conducted analyzing 3,426 articles sourced from 961 publications. Data on research output, collaboration patterns, citation impact, and thematic clusters were extracted and analyzed.
Results. The feld exhibited a robust annual growth rate of 18.42 %, with an average document age of 5.65 years and 26.34 citations per article, indicating high scientifc impact. Collaborative research is prevalent, with 13,598 authors averaging 7.21 co-authors per publication and over 21 % of research produced via international partnerships. Publication formats included journal articles, reviews, and conference papers. Keyword cooccurrence analysis revealed fve main thematic clusters: computational and omics methodologies; tumor biology and immunology; molecular mechanisms and cancer progression; biomarkers and gene regulation; and interdisciplinary cancer research. Publication patterns indicated steady output before 2013 followed by a marked surge peaking near 500 articles in 2023, driven by advancements in genomics, big data analytics, and precision oncology. Citation data highlighted the United States and China as leading contributors, with China leading in publication count through predominantly domestic research, while the United States featured more international collaborations. Other signifcant contributors included Australia, Germany, Canada, and several European and Asian countries.
Conclusion. Research at the intersection of prostate cancer and bioinformatics is rapidly expanding, highly collaborative, and globally distributed. The multidisciplinary and integrative nature of this feld continues to advance understanding, diagnosis, and treatment of prostate cancer through cutting-edge bioinformatics approaches.
CASE REPORTS
Background. Luminal breast cancer, comprising 60–80 % of cases, is characterized by a high frequency of bone metastasis, necessitating continuous surveillance for early detection of distant metastases. Traditional imaging methods have limited sensitivity, especially for small lesions. Therefore, the development of highly sensitive methods for early diagnosis is relevant. Targeted radionuclide imaging of the gastrin-releasing peptide receptor (GRPR) using antagonist-based radiopharmaceuticals, such as [99ᵐTc]Tc-DB8 is a promising non-invasive method for detecting small lesions.
The aim of the study was to demonstrate the potential of [99ᵐTc]Tc-DB8 for detecting bone metastases in patients with luminal breast cancer.
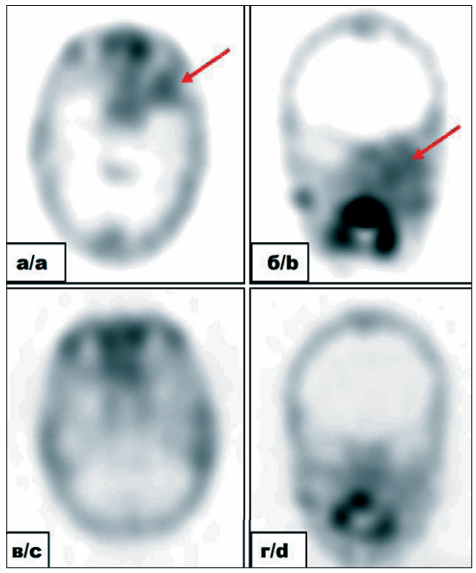
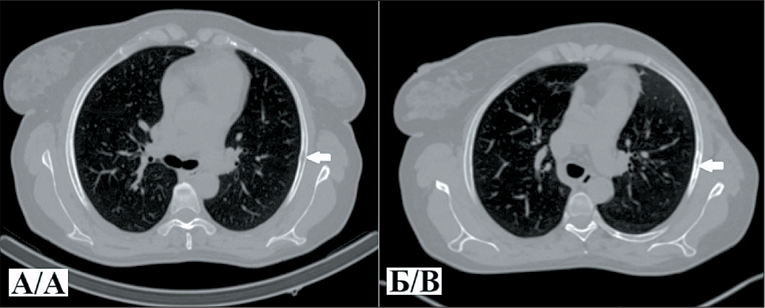
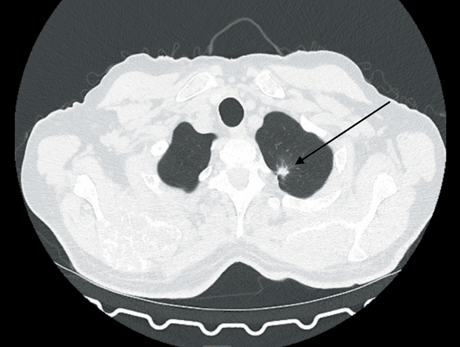
Case report 1. A 51- year-old woman diagnosed with stage IIIC right breast cancer (T2N3M0), with multicentric growth, metastatic involvement of the axillary and subclavian lymph nodes, underwent SPECT/CT 2 hours after the intravenous administration of [99ᵐTc]Tc-DB8 at a protein dose of 80 μg. The detection of a high-uptake [99ᵐTc]Tc-DB8 lesion in the right 5th rib, confrmed as a lytic bone destruction on CT, indicated a high suspicion of bone metastasis. Followup chest CT showed an area of uneven sclerotic changes, interpreted as a response to therapy.
Case report 2. A 42-year-old woman was diagnosed with stage IV right breast cancer (T1N1M1), metastatic involvement of the axillary lymph node, and multiple bone metastases. A SPECT/CT performed 2 hours after the intravenous injection of [99ᵐTc]Tc-DB8 at a dose of 80 μg revealed high uptake of the radiopharmaceutical in the primary tumor, metastatic lymph nodes, and extensive bone metastases. Specifcally, the radiopharmaceutical accumulated in the L2-S2 vertebrae, the right ilium and ischium, and the posterior segment of the 7th rib on the right, identifying these as metastatic sites.
Conclusion. Results of the clinical study on [99ᵐTc]Tc-DB8 demonstrated its high effcacy in detecting bone metastases in patients with luminal breast cancer.
Background. Aggressive angiomyxoma (AA) is a rare mesenchymal neoplasm that predominantly involves the pelvic and perineal regions in women of reproductive age.
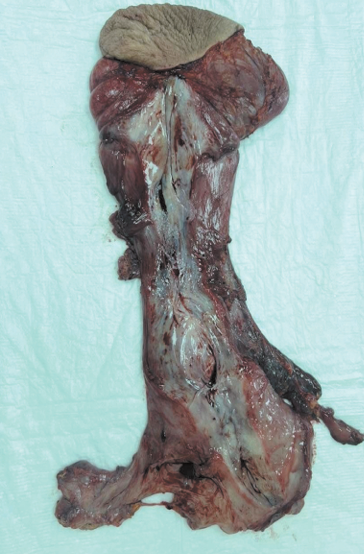
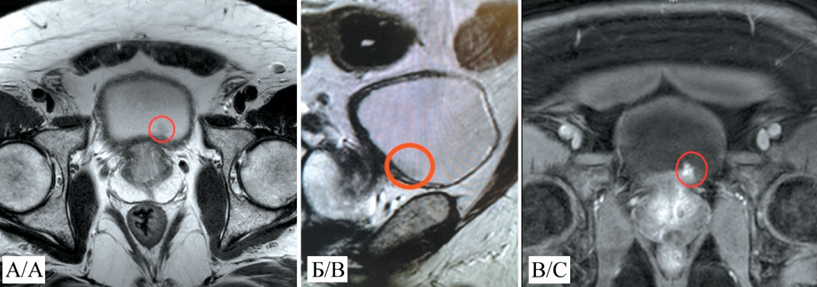
Description of the clinical case. We report the case of a giant 300×160×60 mm AA on the left labia majora in a 41-year-old female patient. The initial differential diagnosis included Bartholin’s gland cyst and inguinal hernia; however, comprehensive examination involving ultrasound, CT, and contrast-enhanced MRI revealed a heterogeneous mass with infltrative growth into the retroperitoneal space. The MRI fndings demonstrated characteristic “layered” changes, and histological examination confrmed the diagnosis: diffuse proliferation of tumor cells within a myxoid stroma, expressing CD34, HMGA2, and estrogen/progesterone receptors. Treatment involved a two-stage surgical procedure: external mobilization of the tumor followed by laparoscopic resection of the retroperitoneal component and pelvic foor defect reconstruction. Histopathological analysis of the resection margins confrmed negative (tumor-free) margins. Lymph node examination revealed no metastases.
Conclusion. MRI is the gold standard for diagnosis of aggressive angiomyxoma, allowing for the assessment of the tumor extent and its relationship with the pelvic foor. The management of aggressive angiomyxoma remains challenging. Radical tumor excision characterized by a high recurrence rate (40–50 %) is shifting toward organ-preserving approaches. Hormonal therapy, combining GnRH agonists with aromatase inhibitors, is an effective strategy to reduce tumor size and recurrence risk. However, this approach is limited by its temporary effect and associated side effects, underscoring the need for a multidisciplinary strategy and further research to standardize treatment and clarify the prognostic role of HMGA2 expression markers for assessing recurrence risks.
Background. Lung cancer is one of the most common cancers worldwide. Most newly diagnosed lung cancer patients present with distant metastases.
Objective: to demonstrate a successful clinical case showing longterm overall and relapse-free survival rates in a patient with disseminated non-small cell lung cancer treated with a combination of immunotherapy and chemotherapy.
Case presentation. A 72-year-old patient diagnosed with stage IV (T1bN0M1b) non-small cell lung asenocarcinoma of the right upper lobe achieved long-term disease stabilization using a combination of atezolizumab, bevacizumab and chemotherapy. The overall and progression-free survival was 38 months with a favorable safety profle.
Conclusion. Despite current drug therapy options, the treatment of metastatic NSCLC remains challenging. This case report demonstrates the effcacy of atezolizumab in combination with bevacizumab and chemotherapy in patients with metastatic, untreated EGFR- and ALK -negative NSCLC negative for programmed cell death ligand 1 (PD-L1).
Background. Bladder cancer is the 10th most common cancer worldwide and the most common malignancy of the urinary tract. Non-muscle invasive bladder cancer accounts for approximately 80 % of cases. Tumors localized in the anterior bladder wall may be challenging to resect completely due to diffcult visual access. Here we present a case of non-muscle invasive bladder cancer localized in a diffcult-to-access area.
Case report. A 67-year-old patient with a mass on the anterior wall of the bladder underwent Nd:YAG laser ablation of non-muscle-invasive bladder cancer of diffcult localization in the urological hospital of the Russian Railways-Medicine Central Clinical Hospital. The previous histological examination of the biopsy specimen of the bladder mass reveled bladder cancer. The superfcial tumor growth was confrmed by preoperative MRI fndings. The Nd:YAG laser with a wavelength of 1064 nm, a power of 40 W and an energy density of 100 J/cm2 was used. The laser beam was delivered through a side fre light guide. After surgery, a two-way catheter was inserted into the bladder for 12 hours. No intraoperative and postoperative complications were detected. Endoscopic evaluation of the effectiveness of the surgical stage was carried out at intervals of 3, 6 and 12 months from the date of surgery. Control cystoscopy revealed no cancer recurrence.
Conclusion. Our clinical case demonstrated the high effcacy and safety of Nd:YAG laser ablation in the treatment of a patient with non-invasive bladder cancer located on the anterior wall of the bladder.
ISSN 2312-3168 (Online)